DOI: 10.20986/resed.2020.3756/2019
ORIGINAL
E-consults, a new tool for pain management. Results of its implementation in an organizational structure of integrated management (EOXI)
Telemedicina, una nueva herramienta para la gestión del dolor. Resultados de su implementación en una estructura organizativa de gestión integral (EOXI)
A. Carregal Rañó1
M. Mayo Moldes1
B. Bustabad Sancho2
1Anestesiología, Unidad de Dolor, Complexo Hospitalario Universitario de Vigo EOXI Vigo, España.
2Atención Primaria EOXI Vigo, España
ABSTRACT
Introduction: On 2014 the Galician Health Service (SERGAS)starts the first teleconsult experience applied to pain unit, and the Sanitary Area of Vigo was chosen for its pilot implementation.
Material and methods: A retrospective longitudinal descriptive study was undertaken during the lapse time January 2015 to December 2018.
Results: In the period of study a total of 2218 teleconsults were requested from the 42 primare care centers of the Sanitary Area. 49% of the teleconsults were preferent. 26% (586) of the requests were rejected and 74% (1632) were evaluated at the Pain Unit. The mean time for response were: 21 days for preferents and 22 for non-preferents.
Conclusions: Teleconsult allows an improvement in the relationship between specialized and primary care levels.
Remarks the importance on consensuated protocols for patient referal. Remarks the need of an updated and well documented portfolio of services.
It allows to correct errors of information transmission between assistance levels and implement correction actions.
Key words: Teleconsultation, e-consult, telemedicine, primary care pain medicine relationship, pain mana-gement
RESUMEN
Introducción: En diciembre de 2014, en el contexto del Plan de Atención del Dolor Crónico del SERGAS, se aplicó la primera experiencia de teleconsultas en unidades de dolor (UD). Se escogió la Estructura Organizativa de Gestión Integrada (EOXI) de Vigo para su aplicación.
Material y métodos: Se realizó un estudio descriptivo longitudinal retrospectivo de todas las teleconsultas enviadas a la UD en el periodo comprendido entre el 1 de enero de 2015 hasta el 31 de diciembre de 2018.
Resultados: Entre enero de 2015 y diciembre de 2018 se han solicitado un total de 2218 teleconsultas. Fueron realizadas desde 42 centros de salud de un total de 42 del EOXI. De las 2218 teleconsultas recibidas, el 49 % fueron preferentes. Respecto a la capacidad de resolución, el 26 % (586) de los pacientes son dados de alta de forma telemática y el 74 % (1632) son citados en la UD.
Los tiempos de respuesta medios para el periodo de tiempo estudiado fueron: 21 días para las teleconsultas preferentes y de 22 para las ordinarias.
Conclusiones: La teleconsulta contribuye a que se conozca y mejore la coordinación entre diferentes niveles asistenciales, evitando derivaciones innecesarias a consulta presencial, mejorando la accesibilidad del paciente y descongestionando los servicios hospitalarios. Pone de manifiesto la importancia de unos protocolos consensuados de remisión y la necesidad de actualizar la información sobre la cartera de servicios. Permite detectar defectos de comunicación entre Atención Primaria y UD. Permite poner en marcha acciones correctoras.
Palabras clave: Teleconsulta, e-consulta, telemedicina, relación con atención primaria al dolor, gestión del dolor
Received: 21-07-2019
Accepted: 16-02-2020
Correspondence: Alfonso Carregal Rañó
alfcarregal@gmail.com
INTRODUCTION
Telemedicine can be defined as the application of information and communication technologies to medicine. Telemedicine development began in the middle of the last century, but it was not until 2 decades ago that it started to be implemented in healthcare systems (1).
Telemedicine is based on the provision of remote medical services, and increasingly, they are part of the service portfolio of many health services. There are several modalities of telemedicine applied in clinical practice such as teleconsultation, telediagnosis, or telemonitoring. Telemedicine is currently used in many clinical specialties and in many healthcare settings, ranging from patient-centric mobile applications to complex interactions between physicians in tertiary hospital reference settings (2). The reasons for deciding to turn to this practice seem to be linked to a high volume of demand for a specific medical service (3).
Telemedicine as a screening and referral system for patients from primary care (PC) to the hospital level is effective not only in pathologies with a high impact due to their severity, but in others that, due to their high prevalence, represent a significant healthcare burden (4,5,6).
There are few studies on the interrelation of primary care through e-consultation with pain units (PU). In this sense, the Canadian group Champlain BASE (Building Access to Specialists through eConsultation) observed a great interest of primary care physicians (PCP) in teleconsultation as a way of relating to PU specialists, praising its bidirectional nature and highlighting the interest of its use for patients with chronic pain attended in primary care (7,8,9,10); The Canadian system, like ours, is characterized by having public management and being universal for citizens in Canada.
Since 1999, the e-interconsultation solutions of the Galician Health Service (SERGAS) allow communication between professionals in health centers (CS) and professionals in hospital centers, facilitating patient access to specialized care. In 2014 and in the context of the Chronic Pain Care Plan, promoted by SERGAS (11), the first pilot experience applied to PU was launched. For its start, the Organizational Structure of Integrated Management (EOXI) of Vigo (Spain) was chosen, which includes, under the same management, the hospital management of the area, the regional hospitals that exist in it and the primary care. Within this EOXI, the PU of the University Hospital Complex of Vigo (CHUVI, Complexo Hospitalario Universitario de Vigo) and its associated primary care centers were selected as a pilot center (11,12). In its initial phase, this experience was only available for a small number of healthcare centers, to later be exported to the entire healthcare area and the rest of Galicia.
Objective
The objective of the present study was to assess whether teleconsultation, after its implementation by SERGAS, is a useful tool for the referral of patients with pain from primary care. Since its implementation, we have not evaluated its effectiveness or the failures or virtues of this referral system.
MATERIAL AND METHODS
A retrospective longitudinal descriptive study was performed.
Scope of study: the Vigo EOXI provides health care to a population of 565,764 inhabitants, of which 20.8 % are over 64 years old and 3.2 % are over 84 years, indicating an aging target population.
Analyzed sample: all teleconsultations sent to the PU from January 1, 2015 to December 31, 2018.
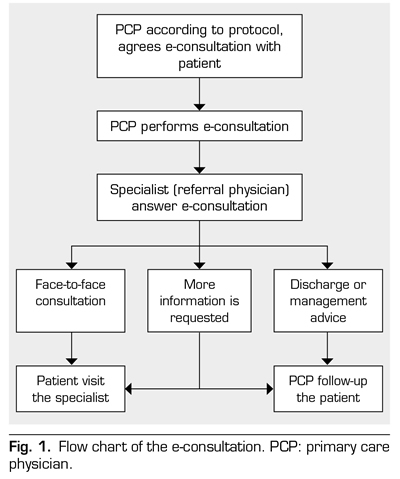
The protocol of all the phases of the teleconsultation is as follows (Figure 1):
1st phase: the patient who attend his/hers primary care center due to severe moderate chronic pain without response to the medical treatment initiated by the PCP will be re-evaluated, and if the patient does not respond satisfactorily, the clinical information of the patient, relevant to the patient’s pain problem and the tried treatments will be completed. PCP consultation requests will be processed exclusively as “Non-face-to-face”.

2nd phase: this form will be evaluated at the PU consultation by the responsible specialists. Then, the specialist will write and send a diagnostic and therapeutic report to the health center. The patient will be scheduled in the corresponding PCP appointment book.
3rd phase: the patient will be scheduled for a visit to the health center, between 3-7 days later, where the patient will be informed by the requesting doctor regarding the result of the report and of the steps to follow; either completing the treatment in the health center, or being referred to our PU if needed.
4th phase: for those patients who need to be referred to the PU, the secretariat of the PU will assume the scheduling and inform the patient.
The priority to assign the appointment of physical presence at the PU will be finally assigned by the specialist physician. There are 2 types of priorities:
Variables analyzed
Number of teleconsultations performed, number of referring healthcare centers, level of priority of the teleconsultations, resolution capacity (proportion of discharges in teleconsultation and patients scheduled in the unit in person) and response time to teleconsultations. The SPSS (r) version 25 program was used to perform the statistical analysis. For the descriptive analysis of the quantitative variables, the mean and standard deviation were used; and for the qualitative variables, the frequency in absolute number and as percentage were calculated.
RESULTS
Teleconsultations conducted during the implementation test phase in 2014 (n = 114) have been excluded from the statistical analysis because the process and platform were adjusted during this period.
A total of 2,218 teleconsultations were requested at the EOXI in Vigo between January 2015 and December 2018 (Figure 2).
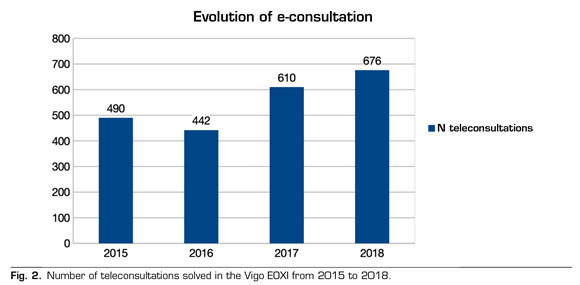
The 42 healthcare centers, which represent the total number of healthcare centers of the EOXI, made teleconsultations to the PU.
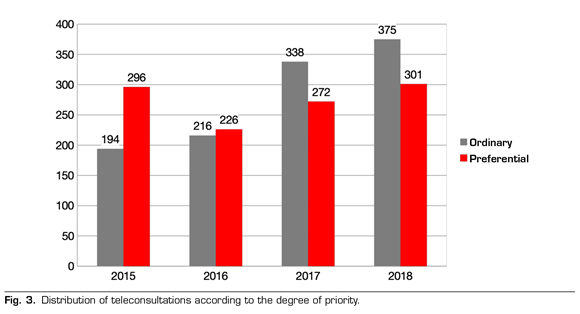
A total of 49 % out of the 2,218 teleconsultations received were preferential. Figure 3 shows the distribution of teleconsultations. A decrease over the years was found, reaching a plateau phenomenon in recent years.
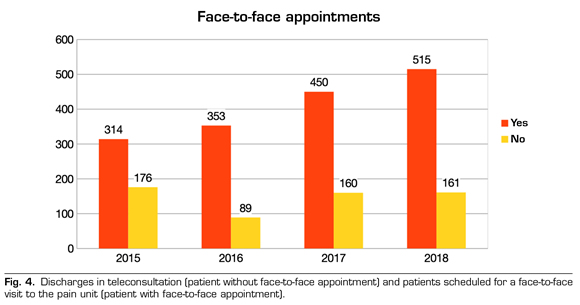
Regarding resolution capacity, Figure 4 shows the distribution of patients per year and the relationship between patients scheduled or discharged. The data indicate that, in total, 26 % (586) of the patients are discharged electronically and 74 % (1632) were scheduled for a visit to the PU for face-to-face assessment. Distributed by years, the percentages were: 36 % (176) of the e-consultations sent were resolved as discharges in 2015, 20 % (89) in 2016, 26 % (160) in 2017 and 24 % (161) in 2018.
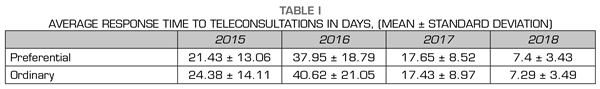
The average response times for the period studied were: 21 days for preferential teleconsultations and 22 for ordinary teleconsultations. When analyzed by years, we obtained the following results: average times for ordinary and preferential teleconsultations in 2015 were 24 days and 21 days, respectively; 41 days and 38 days, respectively, in 2016; 17 days and 18 days, respectively, in 2017; and 7 days for ordinary and preferential in 2018 (Table I).
DISCUSSION
Modern telecommunications in health services allow, in environments of high healthcare demand and where waiting lists are accumulated, to perform an agile, decisive and efficient service, sharing a limited number of resources among a large number of users (13,14).
The explosion of telemedicine in medical practice responds to the decrease in health professionals and the increase in the average age of the population, with the consequent increase in patients with chronic diseases (15,16). Thus, we found that in the Vigo EOXI 20.8 % of its population is over 64 years old and 3.2 % is over 84 years old. The implementation of Teleconsultation in Pain in Galicia began in Vigo on a pilot basis in 2014 and since its beginning until today the number of teleconsultations has been on the rise and it has become generalized in other medical-surgical specialties.
With this study we aimed to explain the telemedicine work performed for 5 years in the PU and to describe the efficacy of this technique based on the variables described in the material.
The efficacy parameters analyzed to assess this potential usefulness have been:
Measurement of the number of teleconsultations received and analysis of their time evolution: The number of teleconsultations received is an important marker in the relationships between different healthcare levels, since it allows us to reliably establish the potential workload that the referral from primary healthcare center (within parameters established in a consensual protocol) will involve for a PU and thus become an objective parameter to establish the technical and human resources necessary to adequately face this burden. The evaluation of this parameter over time indicates, on the one hand, the degree of acceptance as a useful referral tool from the primary care; in theory, the greater the perceived usefulness, the greater the degree of increase in use over time. Furthermore, on the other hand, it allows identifying patterns of variation of the demand, which leads to more objective work planning. The data obtained in our study shows that the number of teleconsultations has increased over time, in our opinion this is an indicator of acceptance. In summary, and from our perspective, the increase in the use of teleconsultations indicates that primary care perceives this tool as useful, and we as receiving agents have more information to plan our activity.
Number of referring healthcare centers: This parameter gives us an assessment of the degree of involvement of the healthcare centers in this new paradigm and it could also be used to indirectly assess the degree of perceived usefulness. The fact that 100 % of healthcare centers have participated in the process, lead us to think that the usefulness of this tool has been perceived as positive.
Priority level of the teleconsultation: As shown in the graphs, the trend since 2015 is a continuous decrease in the proportion of preferential vs. ordinary referrals. This evolution can be justified for several reasons: existence of clear and agreed referral protocols, an improvement in the formation of the PCP, as well as the perception by the latter of the degree of involvement that the receiving PU has regarding the referred patients. Knowledge of the service portfolio can also play an important role in this regard. In this context, we can think, on the one hand, that teleconsultation has helped PCP to better evaluate the referral criteria, and on the other, it has reinforced their confidence in this means of communication because it provides them with quick access to information about their patient, mitigating the mistrust that a system with slow and non-personalized responses can produce. In any case, it will be necessary to continue observing the trend of the data over time in order to establish more definitive conclusions.
Resolution ability: This parameter indicates the proportion of patients scheduled in person compared to those who were evaluated and discharged electronically. This value must be interpreted within the context of having a consensus referral protocol. In theory, and if the protocol is realistic, practically all of the referred patients should be subsidiary to a face-to-face assessment, because previous therapeutic attempts have somehow failed. The data obtained in our study indicates that the rate of patients admitted for physical consultation compared to those rejected has been increasing. We explain this evolution as follows: on the one hand, it seems to us a logical consequence of a consensual protocol, and on the other hand, it reflects the paradigm shift in the treatment of patients with chronic pain, that is, the indication of early interventional technique to minimize the side effects of using centrally acting drugs, especially in aging popu-lations like ours. Furthermore, the application of interventional procedures reduces the global consumption of opioids and thus mitigates the impact that high doses of opioids have generated in countries such as the United States. UU. In our opinion, the fact that the majority of telematically referred patients are assessed in person on an interdisciplinary basis in our pain unit is a reflection of the success obtained with the referral consensus between classes.
Response time to the teleconsultation: The analysis of the data from our work indicates a peak of delay in 2016 that is explained by the exceptional fact that at that time, in our EOXI, the process of merging 2 public hospitals into a new centralized one was performed. This meant the interruption of many healthcare processes throughout the period of fusion and adaptation to new functional situations. From 2016 to the present, the delay time has been decreasing until it reached response values close to 10 days to receive a reply to the teleconsultations made by the PCP. We believe that this parameter is one of the most important to achieve the confidence of PCP in their functioning. In this sense, this decrease in days is positive and reinforces the good dynamic of remission between primary care and our PU. Ideally, they should be 24 h or even less, instantaneous, but this is not possible due to the work dynamics of medical consultations and especially due to the way the circuit is established. We have previously explained that there is a delay since we answer to the teleconsultation until the patient is scheduled to visit the primary care center (between 3-7 days), being difficult to shorten this time.
Since the introduction of teleconsultation in our center, significant advantages from the organizational and healthcare point of view and from the point of view of quality of patient care have been found. An evident improvement in the prioritization of consultations has been achieved, so minimum waiting times have been obtained for preferential patients, such as those with neuropathic or oncological pain. In addition, with this tool we can implement consensual treatments with the PCP and improve pain management until the time of the first visit, and serve as support in the control of patients with chronic pain who have no indication at the current time of an appointment in our pain unit. A fundamental part of all this process is the protocolization of all the phases of the teleconsultation, to achieve a uniform and standardized way of working in all the centers using this service. To maintain this dynamic, it is necessary to periodically perform awareness campaigns to improve the referral system, report changes in the service portfolio and update the protocols.
Strengths of this study
As far as we know, this is the first study published in Spain providing actual figures on the implementation of pain teleconsultation in an EOXI. This study has allowed us to find discrepancies in referrals between PCP and PU, and the need to clearly advertise our service portfolio.
This study can serve as quality control of the evolution of the process in our EOXI and in other areas with characteristics similar to ours, allowing us to observe the evolution of the detected failures.
Weaknesses
We do not have historical figures from our EOXI that allow us to compare our results.
No universally accepted standards with which we could compare our care and delay times are available.
CONCLUSIONS
The teleconsultation contributes to making the coordination between different healthcare levels known and improved, avoiding unnecessary referrals to face-to-face consultation, improving patient accessibility and decongesting hospital services.
The increase detected in the rate of patients admitted for physical consultation shows the importance of a agreed referral protocol between primary care and our PU, and the periodic awareness campaigns of our healthcare center.
It allows to detect communication deficiencies between PCP and PU and to initiate corrective actions.
BIBLIOGRAFÍA